Mammogram
A mammogram is an important screening test used to detect breast cancer. This page explains what a mammogram is, who should have one, what to expect during the exam, and how to understand your results.
Jump to:
What is a screening mammogram?
Why is a mammogram important?
Types of screening mammograms
Mammogram screening recommendations
What to expect during a mammogram
Mammogram results
Mammograms with breast implants
Mammograms while pregnant or breastfeeding
Mammograms and dense breast tissue
Mammogram safety
Mammogram FAQs
What is a screening mammogram?
A screening mammogram is an x-ray of the breast tissue used to look for early signs of breast cancer. It is recommended for women without breast cancer symptoms and is an important part of routine preventive health care. The exam evaluates for abnormalities that are not yet causing symptoms.
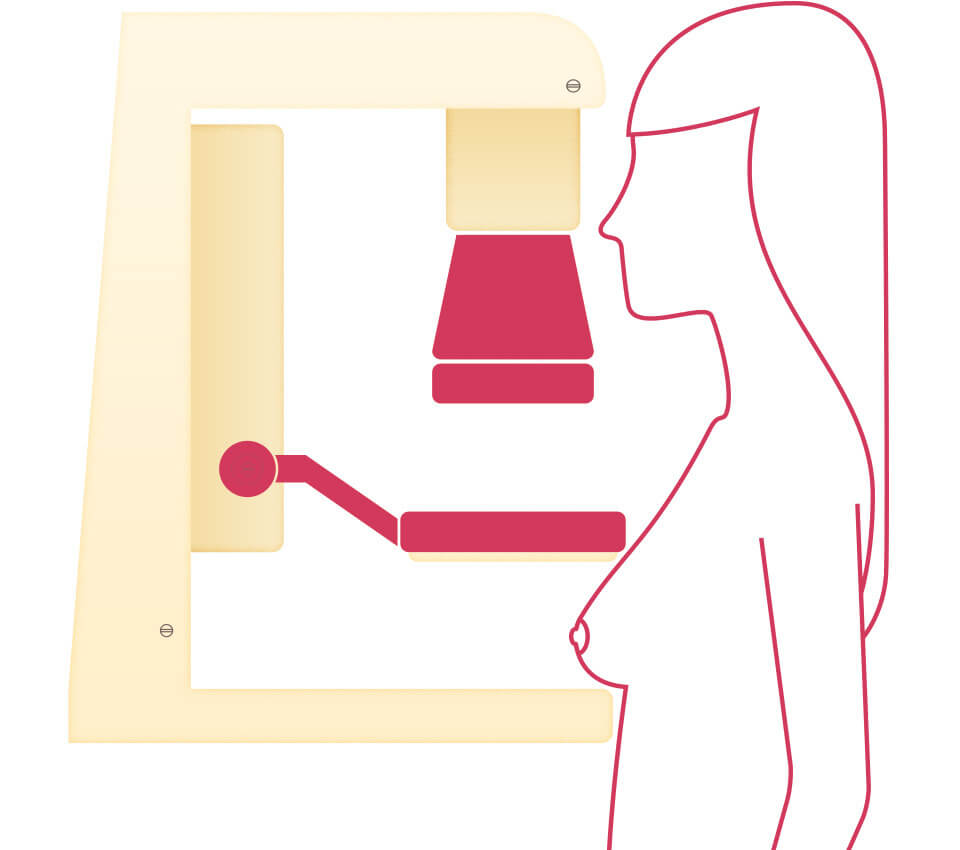
Screening mammograms differ from diagnostic mammograms. Screening mammograms typically include two standard images or views of each breast. Diagnostic mammograms include more views and are used to evaluate breast symptoms such as a palpable lump, breast pain, or to take a closer look at an area in question on your mammogram.
Mammograms use a low dose of ionizing radiation to create detailed images of the breast and help detect abnormalities. Screening mammograms can also detect tiny clusters of calcium deposits called microcalcifications, which may sometimes be an early sign of breast cancer. If an area appears suspicious, a radiologist may recommend additional imaging or a breast biopsy to determine whether cancer or other types of abnormal cells are present.
Mammogram 101
Learn more about mammograms, what to expect before, during, and after your mammogram, and questions to ask your doctor in the free Mammogram 101 guide.
Get the Free GuideWhy is a mammogram important?
Mammograms are one of the most effective tools for detecting early-stage breast cancer, including Stage 0 breast cancer, called ductal carcinoma in situ (DCIS). DCIS often appears as small clusters of calcium deposits, known as microcalcifications, which are best detected with x-ray through mammography. Other breast cancer types can be found on a mammogram as well, such as the most common type of breast cancer, invasive ductal carcinoma.
Studies have shown that women ages 50-74 who receive regular mammography screenings have about a 26% lower risk of dying from breast cancer compared with women who do not get screened, helping save thousands of lives through early detection and treatment before symptoms appear. Early detection increases treatment options, often allows for less aggressive therapies, and is associated with higher survival rates.
Mammograms do not cause breast cancer. The amount of radiation used during screening is very small and is carefully regulated to minimize exposure. Breast compression during a mammogram does not create or spread cancer. The compression helps spread the tissue and holds it still for better images, which also helps reduce the amount of radiation needed for the exam. Research continues to show that the benefits of early detection far outweigh any minimal risks.
Types of screening mammograms
There are two types of screening mammograms: 2D mammograms and 3D mammograms. Both types use low-dose x-rays. The type of mammogram you receive will depend on the facility’s technology capabilities. Your facility may use one or the other, or decide which one is right for you. Mammograms, both 2D and 3D, are widely accessible across the country.
2D mammogram (standard digital)
A 2D mammogram is a standard digital mammogram that takes two x-ray images of each breast, one from the top and one from the side. 2D screening mammograms are considered preventative, and most insurances will cover them at full cost. When verifying insurance coverage, it’s important to make sure that the facility where you are having your mammogram is in-network. It is best to check coverage with your insurance prior to completing your imaging.
3D mammogram (tomosynthesis)
A 3D mammogram, also called digital breast tomosynthesis, takes multiple low-dose x-ray images of the breast from different angles and reconstructs them into thin layers to create a three-dimensional view of the breast tissue. This helps radiologists see better through overlapping tissue, which can improve cancer detection and reduce the chance of being called back for additional imaging. It is especially helpful for women with dense breast tissue.
During the exam, patients remain upright while the breast is compressed, similar to a traditional 2D mammogram. The radiation dose in a 3D mammogram is slightly higher than in a 2D mammogram, but still low and within U.S. Food and Drug Administration (FDA) safety standards. Many insurance plans cover 3D mammography as preventive screening, though coverage can vary. It’s a good idea to check with your insurance provider beforehand.
Need a free or low-cost mammogram?
Through our partner facilities nationwide, NBCF provides free and low-cost mammograms to those in need. Learn more about our National Mammography Program and search for a partner facility in your area.
Find a Free MammogramWho should get a mammogram and how often?
Women of average risk of developing breast cancer should receive an annual mammogram beginning at age 40. Studies show 1 in 6 breast cancers are diagnosed in women in their 40s, and a substantial portion of the lives saved by screening occur in this age group.
However, mammogram age and timing are not a one-size-fits-all approach. Your personal mammogram recommendations should take into consideration your age, personal health history, and other risk factors you may have. For example, women with a family history of breast cancer may need to begin receiving screening mammograms before the age of 40, or receive other screenings, such as breast ultrasound or MRI, in addition to an annual mammogram. Talk with your doctor about the breast cancer screening schedule that is right for you.
Screening recommendations by age and risk
Age & Risk | Recommendation |
40+, average risk | Annual screening mammogram |
40+, increased or high risk | Annual screening mammogram plus additional screenings, such as ultrasound or MRI; discuss with your healthcare provider |
Under 40, average risk | No annual screening mammogram until age 40; monthly breast self-exam recommended |
Under 40, increased or high risk | May start screenings earlier than 40, depending on risk; discuss with your healthcare provider |
Any age with symptoms | Diagnostic mammogram and possible other imaging; discuss with your healthcare provider right away |
When to start screening earlier (high-risk situations)
Some women who have increased breast cancer risk factors should start screening mammography earlier than age 40. Risk factors to discuss with your doctor about earlier screening include:
- Family history of breast cancer, particularly a first- or second-degree relative on either the mother’s or father’s side
- Testing positive for a BRCA or other genetic mutation
- Dense or extremely dense breast tissue
- Prior radiation to the chest (chest or mantle radiation therapy at a young age from Hodgkin lymphoma, for example)
- Starting menstruation early, before age 12
- Late childbearing age of first child
- Late menopause age, after 55
- Nulliparity (no biological children)
- Ashkenazi Jewish heritage
- History of abnormal breast biopsy
Healthcare providers may use a risk assessment tool, such as the Tyrer-Cuzick Model, to help create a personalized screening plan. By entering information about your personal and family history, the tool estimates your 10-year and lifetime risk of developing breast cancer compared to the general population. A lifetime risk of 20% or higher is considered high risk.
If your risk falls within this range, your provider may refer you to a breast specialist or work with you to develop a more personalized screening and risk-reduction plan. This may include additional screening, such as breast MRI, discussing whether genetic testing is appropriate, and reviewing lifestyle changes or other strategies that may help lower your risk.
What to expect during a screening mammogram
A bilateral screening mammogram takes two views of each breast, totaling four views. A screening mammogram is a quick outpatient exam that only takes about 15-20 minutes to complete. However, plan to spend approximately 30-45 minutes at the facility in total. This includes check-in, signing any necessary documentation, and changing into a gown that opens in the front. You will only need to remove clothing from the waist up, so be sure to wear a two-piece outfit.
During the exam, the mammogram technologist will carefully position your breast on the imaging plate, which applies firm compression for a few seconds while each image is taken. You may be asked to adjust your head or turn your shoulders slightly to help capture the clearest view of the breast tissue. At times, you may also be asked to hold your breath briefly while the x-ray is taken to prevent motion blur.
You may feel some temporary discomfort during compression, but it lasts only a few seconds. Compression is important because it spreads out the breast tissue, allowing for clearer images of the entire breast while using the lowest radiation dose possible.
There are a few ways to make the experience more comfortable:
- Schedule your mammogram 7 days after your menstrual period, when your breasts are the least tender.
- Take an over-the-counter pain reliever, such as acetaminophen or ibuprofen, about 30-60 minutes before your appointment, if needed.
- Let the technologist know how you’re feeling. They can often adjust positioning and will do their best to make you as comfortable as possible
How to Prepare for a Mammogram
Read How to Prepare for a Mammogram for more information about what to expect before, during, and after a mammogram. Plus a checklist to help you prepare.
Read the Blog PostMammogram results
Waiting for mammogram results can feel stressful, and that’s completely normal. Most mammogram results are normal, and being called back for additional imaging is common and does not necessarily mean cancer is present.
How long does it take to get mammogram results?
If you’ve had breast imaging at another facility in the past, make sure those prior images are available for your current appointment. You may need to request that the previous imaging center send them electronically or provide a disc for you to bring. Having prior studies allows the radiologist to compare images over time, which can help avoid delays and may reduce the need for additional imaging.
At most imaging centers, screening mammograms are read, or interpreted, within 1-3 business days. Some facilities, particularly high-volume centers or those waiting on prior images, may take up to 1-2 weeks.
If you have been waiting more than a week, it’s reasonable to contact the imaging facility to check on the status of your results. Many patients receive their results through an online patient portal through the provider who ordered the mammogram, or by letter in the mail.
What does a normal mammogram result mean?
A normal screening mammogram means no findings were identified that require additional testing, and you can return in one year for your next routine screening. In some cases, an area may be seen on the mammogram but is determined to be benign or stable when compared with prior images.
Out of every 100 women who have a mammogram, about 90 receive normal results. Around 10 are asked to return for additional testing.
What happens if my mammogram results are abnormal?
If you are called back due to abnormal findings on a screening mammogram, the imaging facility will let you know that additional imaging is needed.
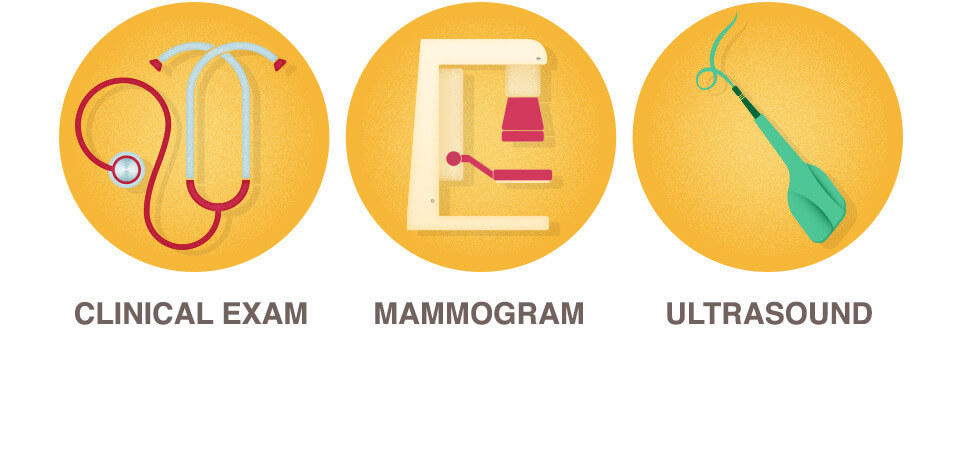
Most often, this means a diagnostic mammogram, which takes more detailed, magnified views of the area in question. A breast ultrasound is also commonly performed to get more information. In some cases, if the area still isn’t fully clear, a breast MRI may be recommended for further evaluation.
It’s important to remember that even among those who undergo a breast biopsy due to an abnormal mammogram finding, about 80% of biopsy results are benign (non-cancerous). A breast biopsy is a procedure in which cells are removed from a suspicious area to check for cancer.
Abnormal Mammograms & What to Do Next
If you’ve had an abnormal mammogram, download this free list of specific questions to ask your doctor at your next appointment. Be prepared to understand your results and empowered with critical information about your next steps.
Get the Free GuideMammograms in special situations
If you have breast implants, are pregnant, or are breastfeeding, you may be wondering whether a mammogram is still right for you. In most cases, it is. Be sure to let your healthcare provider and the mammogram technologist know your situation ahead of time so the radiology team can plan appropriately and answer any questions you may have. Scroll below to find the section that applies to you.
Mammogram with breast implants
Having a mammogram with saline or silicone breast implants is safe. However, be sure to let the technologist know you have implants before your exam.
In many cases, the technologist will use a special positioning method called the implant displacement technique (also known as the Eklund technique). During this process, the implant is gently moved back toward the chest wall while the natural breast tissue is brought forward and compressed separately. Having implants may require a few extra images, which allows the radiologist to see as much natural breast tissue as possible.
Mammogram during pregnancy
If you are pregnant, you may wonder whether you should still have a screening mammogram. The radiation in mammograms is far below levels known to cause harm to a developing baby. Additionally, imaging approaches may be adjusted to protect both the mother and fetus. However, because breast cancer during pregnancy is uncommon, the National Cancer Comprehensive Network guidelines note that routine screening is often postponed until after delivery for women at average risk.
However, breast symptoms during pregnancy should not be ignored or delayed, as pregnancy-associated breast cancer can occur. If you notice a new lump while pregnant, contact your healthcare provider right away.
Mammogram while breastfeeding
Breast imaging during lactation (breastfeeding) is very similar to breast imaging in women who are not breastfeeding. Emptying the breasts by breastfeeding or pumping before the exam may help reduce breast density and improve image quality.
Mammograms and dense breast tissue
Every breast has a different mixture of breast tissue. Breast tissue may be referred to as non-dense (more fatty) and dense (less fatty with more fibroglandular tissue). Dense breast tissue means there is more fibroglandular tissue.
Nearly 50% of women age 40 and older have dense breast tissue. Breast density is determined by the radiologist reading your mammogram. It is included in your mammogram report.
Breast tissue is categorized into one of four groups:
- Predominantly fatty
- Scattered fibroglandular density
- Heterogeneously dense
- Extremely dense
On a mammogram, fatty (non-dense) tissue appears dark, while fibroglandular (dense) tissue appears white. Because abnormalities such as tumors also appear white on a mammogram, dense breast tissue can make mammograms more difficult to interpret, as areas of concern may blend in with normal dense tissue.
Dense breasts do not mean you have a problem; it is a common and normal finding. However, breast density can affect how a mammogram is interpreted and may influence screening recommendations for some women.
Federal regulations now require all mammogram facilities in the United States to inform patients whether their breasts are considered “dense” or “not dense.” This information is included in the written summary you receive after your mammogram, often sent by mail. The purpose of this notification is for you and your provider to determine if you need additional breast screening in addition to your mammogram.
Dense Breasts Q&A Guide
According to the National Cancer Institute, nearly 50% of all women age 40 and older have dense breasts. This free guide answers frequently asked questions about dense breasts so you can be your own best advocate for your health.
Get the Free GuideWhat if I have dense breast tissue?
Many women with dense or extremely dense breast tissue need supplemental breast cancer screening beyond an annual mammogram. Breast MRI with and without contrast is recommended for these women at higher-than-average risk of breast cancer. Breast MRIs generally require prior authorization from your insurance. The MRI takes about 25 minutes. If an MRI cannot be performed, a bilateral whole breast ultrasound may be ordered instead. Talk with your provider about which supplemental screening option is right for you.
Mammogram safety
It is completely normal to have concerns about radiation, especially before your first mammogram. You can feel confident knowing that mammography is a safe and important tool for protecting your health.
Are mammograms safe?
The amount of radiation used during a screening mammogram is very low, and the benefits of early detection far outweigh this minimal exposure. The radiation dose in a mammogram is similar to what you might receive during a transatlantic flight. The American College of Radiology also notes that a single mammogram is comparable to about 26 days of natural background radiation from everyday life.
Mammograms do not damage breast tissue or cause breast cancer to spread. The compression used during the exam may feel uncomfortable, but it does not injure the breast or “push” cancer cells into other areas of the body. The pressure is brief and controlled, and it is necessary to spread out the breast tissue so clearer, more accurate images can be taken.
Frequently asked questions about mammograms
What does a mammogram show?
A mammogram is an x-ray that shows normal and abnormal findings within the breast tissue.
Why start mammograms at age 40?
Large screening trials showed that mammography in women in their 40s reduced death from breast cancer.
What is a bilateral mammogram?
Bilateral means both sides. A bilateral mammogram is a mammogram of both the left and the right breasts.
What is the difference between a screening and a diagnostic mammogram?
A screening mammogram is a routine standard mammogram used for annual detection. A diagnostic mammogram is a mammogram with additional magnified views to further investigate a possible area of concern.
Can I get a mammogram if I have breast impalants?
Yes, you can safely have a mammogram if you have breast implants. Be sure to tell the technologist beforehand, as special imaging techniques can be used to see as much natural breast tissue as possible.
Can I get a mammogram while pregnant or breast feeding?
Yes. However, talk to your doctor. If you are pregnant, screening is often postponed in average-risk women. Protective shielding can be used if imaging is needed. While breastfeeding, nursing or pumping beforehand can help make the images easier to interpret.
What does an abnormal mammogram mean?
An abnormal finding or abnormal result on a mammogram means an area on your breast needs a closer look with additional imaging, such as a diagnostic mammogram and/or a breast ultrasound. Callbacks due to abnormal findings are common, especially after your first mammogram, when there are no others to compare to. Most women who are called back for additional screening do not have breast cancer.
Sources:
National Cancer Institute
Centers for Disease Control and Prevention
American Society of Breast Surgeons
American College of Radiology
American Society of Breast Imaging
American College of Radiology



