Mastectomy
What is a mastectomy?
A mastectomy is a surgical procedure to remove all or most of the breast tissue. The purpose of a mastectomy is to remove cancer from the breast or to significantly lower the chance that breast cancer will develop or return.
Mastectomies are an important treatment option for many people diagnosed with breast cancer and may be recommended depending on the size, location, or type of cancer. In some cases, individuals with a strong family history or certain genetic mutations may also consider a preventive mastectomy, also called a prophylactic mastectomy, to help lower their future risk of developing breast cancer.
In the past, breast cancer surgery often required removing the entire breast, chest wall, and all axillary lymph nodes in a procedure called a total radical mastectomy. Today, less severe surgery options exist and are common.
If the cancer is detected early enough, there are usually surgical options that will remove the cancer while preserving breast tissue. The common options are a lumpectomy (most often followed by breast radiation treatments), a partial mastectomy, and a simple mastectomy.
Jump to:
What is a mastectomy?
Mastectomy vs. lumpectomy
Common mastectomy procedures
Reasons for a mastectomy
Stages and types of breast cancer that require a mastectomy
The mastectomy procedure
Other treatments before or after a mastectomy
Mastectomy risks and complications
Breast reconstruction after a mastectomy
Breast cancer recurrence after mastectomy
Life after mastectomy
Latest in mastectomy technology
Mastectomy vs. lumpectomy
Both a lumpectomy and a mastectomy are surgical procedures used to locally treat breast cancer. A lumpectomy removes the cancer, along with a small margin of surrounding healthy breast tissue, while preserving most of the breast. A mastectomy removes the entire breast and most of the breast tissue.
In women with early-stage breast cancer, studies have shown that lumpectomy followed by radiation therapy can provide survival outcomes similar to mastectomy. The best option depends on factors such as the size and location of the tumor, breast size, genetic risk, and patient preference.
A mastectomy may involve removing one breast (a unilateral mastectomy) or both breasts (a bilateral, or double, mastectomy).
It is important to know that having a mastectomy does not necessarily result in longer survival than having a lumpectomy followed by radiation. Both approaches are effective in treating breast cancer. Your oncology team will help you determine which type of procedure is best for you.
Breast Cancer Surgery Guide
This free guide shares details on surgical options, helpful terms to know, information on reconstruction and cosmetic options, and support for healing from surgery. Plus, hear a Q&A from two-time breast cancer survivor and medical expert, Lillie Shockney.
Get the Free GuideCommon mastectomy procedures
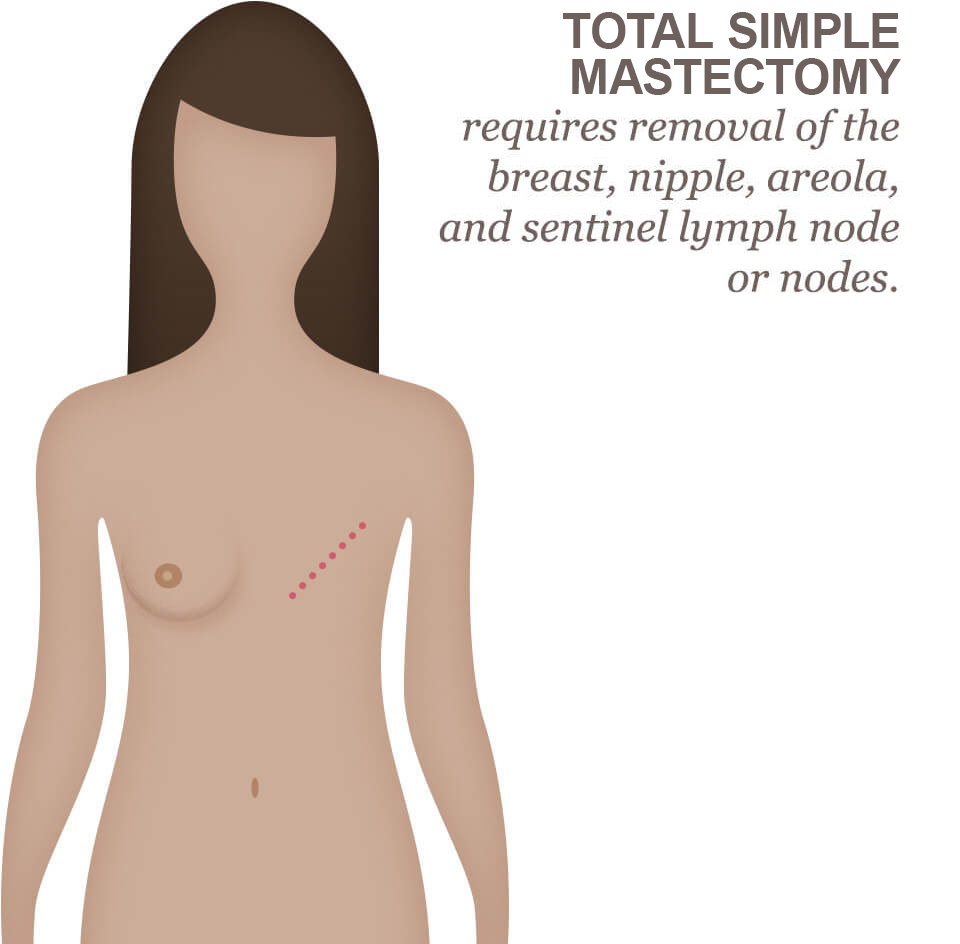
Total simple mastectomy
A total simple mastectomy involves the removal of the entire breast. This includes the breast tissue, nipple, areola, and, in some situations, the sentinel lymph node(s). This type of mastectomy removes the breast skin as well.
Skin-sparing mastectomy
This procedure requires the removal of most of the breast tissue, nipple, areola, and, in some situations, the sentinel lymph node(s), but it does not remove the skin.
Many women who intend to have breast reconstruction will opt for this procedure. During the procedure, the breast tissue is removed while the skin envelope is preserved, allowing your surgeon to reconstruct the breast using an implant or tissue from another part of the body, such as the abdomen, buttocks, or inner thigh. Using your own natural tissue is called autologous tissue reconstruction.
Nipple-sparing mastectomy
A nipple-sparing mastectomy is similar to a skin-sparing mastectomy but preserves the nipple and areola (known together as the nipple-areola complex) as well as the breast skin. During this procedure, the breast tissue is removed while the skin, nipple, and areola remain intact.
Not all patients are candidates for this approach; your surgeon will evaluate the tumor’s location and other factors to determine whether it is safe to preserve the nipple-areola complex. Incisions are often placed in less visible areas, such as under the breast along the inframammary fold (the natural, skin-to-chest attachment underneath the breast), although incision placement can vary.
Modified radical mastectomy
This procedure involves the removal of the entire breast, including the nipple and areola, along with most axillary (nearby) lymph nodes. However, the chest wall muscles are preserved.
Radical mastectomy
This is the most extensive type of mastectomy, as it involves the removal of the entire breast, breast tissue, skin, nipple, areola, chest wall muscles, and axillary lymph nodes. In the early 1970s, this was considered the standard surgical treatment for breast cancer. Today, it is rarely performed and is typically reserved for situations when an aggressive tumor has invaded the chest wall muscles.
Prophylactic (preventive) mastectomy
A prophylactic mastectomy, also known as a risk-reducing or preventive mastectomy, is performed before breast cancer has been diagnosed. It removes one or both breasts to significantly reduce someone’s risk of developing breast cancer by about 90–95%. It is often considered for people at a very high risk of breast cancer, such as those with certain inherited genetic mutations, including BRCA1 or BRCA2, or a strong family history of the disease.
A prophylactic mastectomy significantly reduces the risk of breast cancer; however, it does not eliminate it entirely, as small amounts of breast tissue may remain.
Reasons for a mastectomy
Breast cancer
Mastectomy is indicated for patients who are not candidates for breast conservative therapy (lumpectomy) or for those who choose a mastectomy over a lumpectomy for preference. For patients with early-stage invasive breast cancer (Stage 1 or Stage 2) who still have cancerous cells left after a lumpectomy, doctors may recommend either another surgery to remove more tissue, called a re-excision, or a mastectomy to remove the whole breast. Mastectomy is also often chosen when there is widespread disease (disease that involves two or more quadrants of the breast). It is also used when there are multiple breast cancer tumors in the breast, known as multicentric disease.
Prevention in high-risk patients
A prophylactic (preventive) mastectomy, undertaken before breast cancer is diagnosed, removes most breast tissue and can reduce the risk of developing breast cancer by about 90-95%. A small amount of breast tissue may remain, so the risk is greatly reduced but not completely eliminated. Because very little breast tissue remains, routine screening with mammograms or breast MRI is often no longer recommended after a bilateral prophylactic mastectomy. However, regular follow-up with a healthcare provider and attention to any new changes in the chest wall or skin are still important.
Phyllodes tumors
Phyllodes tumors are rare tumors of the breast, accounting for less than 1% of all breast tumors found in women aged 40-50. Most phyllodes tumors are benign (non-cancerous), but can recur (come back) about 60-75% of the time. One in four phyllodes tumors will be malignant. Reasons for a mastectomy due to phyllodes tumors include malignancy (cancer), large tumor size, need for wider margins around the tumors, and recurrent tumors.
Gynecomastia
Gynecomastia is a benign condition that causes enlargement of breast tissue in males. In some cases, surgery to remove the excessive breast tissue may be performed, particularly if the enlargement is bothersome or does not improve. Although this procedure is different from a mastectomy performed for breast cancer, it also involves the removal of breast tissue.
Stages and types of breast cancer that require a mastectomy
For many early-stage breast cancers, patients may choose between a lumpectomy followed by radiation therapy, called breast-conserving therapy, or a mastectomy. Large clinical trials have shown that breast-conserving therapy provides survival outcomes equivalent to mastectomy for early-stage breast cancer. However, when Stage 0 ductal carcinoma in situ (DCIS) involves a large portion of the breast or is present in multiple areas, a mastectomy may be recommended to ensure all of the affected tissue is removed.
In Stage 1 and Stage 2 breast cancer, tumors are typically smaller and confined to the breast or nearby lymph nodes. Many patients choose a lumpectomy followed by radiation therapy, although mastectomy may still be recommended depending on the size of the tumor relative to the breast, the presence of multiple tumors, or personal preference.
In Stage 3 breast cancer, the cancer may have spread to nearby lymph nodes or surrounding tissues but has not spread to distant organs. Treatment often begins with neoadjuvant chemotherapy, which is given before surgery to shrink the tumor. After this treatment, surgery is performed, and a mastectomy is often recommended to remove the remaining cancer, although in some cases, a lumpectomy may still be possible depending on the response to treatment.
Mastectomy may be recommended when a lumpectomy is not the best option. This can occur when the tumor is large relative to breast size, when multiple tumors are present, when clear surgical margins cannot be achieved, or when the cancer does not respond adequately to treatment (chemotherapy) before surgery. It may also be recommended for certain situations, such as inflammatory breast cancer, extensive suspicious calcifications in DCIS, recurrence after prior lumpectomy and radiation, or when radiation therapy is not recommended.
Some people choose mastectomy to reduce future cancer risk, particularly those with genetic mutations or prior chest radiation. Younger patients with more aggressive breast cancers may also prefer mastectomy. The specific type of mastectomy depends on factors such as tumor location, breast size and shape, cancer type, lymph node involvement, and whether reconstruction is planned, and is determined together with your surgical team.
The mastectomy procedure
A mastectomy is performed in the operating room while you are under general anesthesia, which means you will be asleep during the procedure. While the exact steps can vary depending on the type of mastectomy and whether reconstruction is planned, most surgeries follow a similar process.
First, the surgical team cleans the skin and gives antibiotics through an IV to help prevent infection. The surgeon then makes an incision on the breast, with the location depending on the type of mastectomy being performed. The breast tissue is carefully removed. Depending on the procedure, the nipple, areola, or some surrounding skin may also be removed.
In many cases, the surgeon will also evaluate the lymph nodes in the underarm to see if cancer has spread. This may involve removing one or a few lymph nodes for testing, which can slightly increase the risk of swelling in the arm, known as lymphedema. If needed, your surgeon can refer you to a lymphedema therapist for prevention strategies or treatment.
If there is no evidence of lymph nodes containing cancer when imaging studies are done, then a procedure called sentinel node biopsy is done. The breast is injected with a radioactive isotope or blue dye that travels from the breast tumor to the lymph nodes under the arm. The first lymph node that turns blue is the sentinel node. Just this node is then removed and tested to see if any cancer cells are present.
If you choose immediate breast reconstruction, it may be started during the same surgery as your mastectomy. This is typically performed by a plastic (reconstructive) surgeon, though in some cases, a single surgeon may perform both procedures.
Reconstruction options include placing a temporary tissue expander or an implant at the time of surgery. Another option uses your own tissue (autologous reconstruction), such as a DIEP or TRAM flap from the abdomen, or a latissimus flap from the upper back.
Surgical drains are usually placed to remove fluid as you heal. You will be asked to track the output of these drains at home so your surgeon can determine when they are ready to be removed, typically within 1-2 weeks after surgery, though sometimes longer.
Most mastectomy incisions are closed with dissolvable sutures and covered with steri strips to support healing. Your surgeon will let you know when it is safe to remove dressings or wraps and when you may begin showering.
It is common to feel tightness, numbness, or pulling across the chest as you heal. You will have lifting restrictions and should avoid strenuous activity involving the upper and lower body while recovering. Wearing a supportive bra after surgery is helpful. Driving should be avoided until you are no longer taking prescription pain medication, all drains are out, and until your surgeon says it is safe. Swimming and bathing should also be avoided until you are cleared by your surgeon. Showering is usually allowed.
Breast reconstruction procedure
If you choose immediate breast reconstruction, it may be started during the same surgery as your mastectomy. This is typically performed by a plastic (reconstructive) surgeon, though in some cases, a single surgeon may perform both procedures.
Reconstruction options include placing a temporary tissue expander or an implant at the time of surgery. Another option uses your own tissue (autologous reconstruction), such as a DIEP or TRAM flap from the abdomen, or a latissimus flap from the upper back.
Checklist for Recovery After Mastectomy
Learn about the 17 must-haves for mastectomy recovery, recommended by patients and survivors themselves.
Read the Blog PostOther treatments before or after a mastectomy
Radiation
In some cases, having a mastectomy may mean that radiation therapy is not needed. Radiation therapy uses high-energy beams to destroy cancer cells. However, radiation is typically recommended after a lumpectomy to make it as effective as a mastectomy in preventing cancer recurrence. In select situations, radiation after a lumpectomy may be safely omitted based on factors such as the patient’s age, tumor characteristics, and overall health.
Radiation may still be recommended after a mastectomy if cancer is found close to the edge of the removed tissue, if lymph nodes are involved, or if the tumor is large or more advanced.
Chemotherapy
Chemotherapy may be given before surgery, called neoadjuvant chemotherapy, to shrink the tumor. This is often used for larger tumors, lymph node involvement, or more aggressive cancers such as HER2-positive or, in some situations, triple-negative breast cancer (TNBC). Chemotherapy may also be recommended after surgery (adjuvant chemotherapy) based on final pathology results.
Hormonal therapy
Hormonal therapy may be used for hormone receptor-positive cancers to lower estrogen levels or to block its effects and reduce the risk of recurrence. Hormonal therapy is usually taken for a period of 5-10 years.
Mastectomy risks and complications
As with any surgery, there are potential risks and complications. These may include:
- General anesthesia: Reactions to anesthesia are uncommon but can occur with any surgical procedure. Your care team will review your medical history beforehand and, in some cases, may order preoperative clearance or additional testing to make sure it is safe for you to undergo anesthesia.
- Infection: All surgeries carry a risk of infection. Watch for signs such as fever, redness, warmth, swelling, or drainage that is cloudy or has a foul odor.
- Seroma: A seroma is a collection of fluid that can build up in the surgical area. Small seromas often resolve on their own, while larger or uncomfortable ones may need to be drained.
- Hematoma: A hematoma is a collection of blood that can cause swelling, pain, or bruising. Most resolve on their own, but larger hematomas may require treatment.
- Lymphedema: Lymphedema is swelling that can occur in the arm, chest wall, breast, or back due to changes in lymphatic drainage after lymph node removal.
- Cording (axillary web syndrome): A tight, cord-like structure that can develop under the arm and sometimes extend down the arm. Physical or occupational therapy can help relieve tightness and restore range of motion.
- Post-mastectomy pain syndrome: Nerve-related pain that may persist after surgery, sometimes described as burning, tingling, or shooting discomfort. This type of pain can develop months after surgery and, in some cases, may last for years. Symptoms can vary in intensity, and your care team can help manage this with medications, therapy, or other supportive treatments.
- Tissue necrosis: A rare complication where reduced blood supply causes skin or tissue to break down. This may appear as dark or blackened tissue and may require treatment. Smoking can increase this risk.
- Fat necrosis: A benign (non-cancerous) condition where fatty tissue is damaged and forms a firm lump or oil cyst. These often resolve on their own and typically do not require treatment.
- Phantom breast pain or sensation: Sensation that feels as though the breast is still present, as well as tingling, itching, pressure, or pain in the area where the breast was removed, may be known as phantom breast pain. This occurs due to nerve changes after surgery. It is common and often improves over time.
- Emotional impact: The emotional impact of a mastectomy is important to consider and should be discussed before surgery. It is normal to experience a range of emotions, including sadness, anger, anxiety, or uncertainty related to your diagnosis, changes in body image, or recovery. You are not alone in feeling this way, and support is available. Connecting with your care team, loved ones, a counselor, or a support group can be an important part of healing.
Emotional Support Workbook
Breast cancer patients and survivors face unique emotional challenges. The free Emotional Support Workbook for Breast Cancer Patients & Survivors can help you move from emotional pain to emotional healing.
Get the Free WorkbookBreast reconstruction after a mastectomy
After a mastectomy, some women choose to have breast reconstruction, while others do not. If you decide not to have reconstruction, you may choose an aesthetic flat closure, where the breast tissue is removed and the chest is contoured to lie flat.
Immediate breast reconstruction is performed at the same time as the mastectomy, during the same surgery. This means a breast shape is created right away using either an implant or tissue from another part of the body.
If choosing implants, saline and silicone implants are both safe options. Saline implants are filled with sterile salt water and have a firmer texture, while silicone implants are filled with a gel that feels more soft.
Delayed reconstruction is performed at a later time, after you have healed from the mastectomy. This approach may be recommended if additional treatments, such as radiation therapy, are needed or if you prefer to wait.
The timing of reconstruction depends on your overall treatment plan, recovery, and personal preference, and is decided together with your surgical team.
Not everyone is a candidate for breast reconstruction, but many women are. In general, good candidates are those in overall good health without medical conditions that could interfere with healing. Certain factors may increase the risk of complications, including uncontrolled diabetes, obesity, and smoking. Your surgical team will consider these factors when discussing whether reconstruction is a safe and appropriate option for you.
Breast cancer recurrence after mastectomy
After a mastectomy, it is uncommon but still possible for breast cancer to return. Recurrence may occur in the chest wall, skin, or nearby lymph nodes, so it is important to be aware of any changes. Watch for new lumps or nodules under the skin, thickened areas, or changes in color near or along your scar. Many of these changes are related to scar tissue, but should always be evaluated by your healthcare provider.
Breast cancer can recur in different ways:
- A local recurrence occurs in the same area as the original cancer, such as the chest wall or surgical scar.
- A regional recurrence involves nearby lymph nodes, the tissue around the clavicle, or the lymph nodes near the clavicle.
- A distant recurrence means the cancer has spread to other parts of the body.
What You Need to Know About Breast Cancer Recurrence
This free eBook, written by breast cancer expert Lillie Shockney, RN., BS., MAS, ONN-CG, will help you understand what recurrence is, signs and symptoms to be aware of, hormonal therapy, and more.
Get the Free eBookCertain types of breast cancer, such as invasive lobular carcinoma (ILC), can sometimes be more difficult to detect and may have patterns of recurrence that are less obvious, which makes ongoing follow-up especially important.
The risk of recurrence varies based on the stage and type of the original cancer, as well as the treatments received. In general, early-stage breast cancer has a relatively low risk of recurrence with appropriate treatment, while Stage 2 and 3 cancers carry a higher risk. These estimates are based on large groups of patients and do not predict an individual’s risk.
Life after mastectomy
Mastectomy has been associated with changes in sexual health and intimacy. Data suggest that approximately 42% of women experience some degree of sexual dysfunction following surgery. Compared to breast-conserving (lumpectomy) approaches, mastectomy, particularly without reconstruction, is more likely to be associated with changes in breast-related intimacy.
For example, before surgery, about 87% of women reported that their breasts played a role in intimacy. After a mastectomy, this decreased to about 59%, suggesting that some women experience changes in how their chest contributes to intimacy. In contrast, women who undergo reconstruction report higher rates of preserved intimacy (approximately 76% after surgery). Additionally, satisfaction with breast appearance after surgery, reported by about 65% of women who undergo reconstruction, is associated with better sexual well-being.
These changes can be complex and deeply personal, and they may evolve over time. Open conversations with your care team and partner, along with support resources, can help you navigate intimacy and sexual health after surgery.
Sexual Health and Breast Cancer
Learn how breast cancer treatment can affect your sexual health and how you can reconnect with your body and partner in Sexual Health and Breast Cancer: A Healing, Intimacy, and Hope Guide.
Read the Blog PostAfter a mastectomy, some women may struggle with body image, including feeling less feminine. Physical changes, such as loss of sensation in the breast or nipple, scarring, discomfort, or difficulty finding comfortable positions, can also impact sexual health. These experiences are common but are often underaddressed.
Latest in mastectomy technology
There are increasing advances in nipple-sparing mastectomy techniques, which preserve the nipple-areola complex and as much healthy skin as possible, allowing for a more natural reconstruction outcome in appropriately selected patients.
Even with these refined approaches, challenges such as scarring, changes in sensation, and reduced blood flow to the skin can still occur. Newer techniques, including robotic-assisted nipple-sparing mastectomy, aim to address these challenges through smaller incisions, gentler tissue handling, and improved visualization during surgery, which may support better cosmetic outcomes and tissue preservation.
Additional innovations include nerve-preserving reconstruction, minimally invasive surgical approaches in select centers, and improved implant placement techniques. Some of these advances are becoming more widely available, while others are still evolving and may not be offered at every hospital.
Sources
American Cancer Society
National Comprehensive Cancer Network (NCCN)
National Institutes of Health
American Cancer Society
American Society of Breast Surgeons
American Society of Breast Surgeons
American Journal of Managed Care
Mayo Clinic



